Comprehensive analysis of neurological disease patterns in a fragile health system in Somalia
This study, conducted at Somalia’s largest referral and teaching hospital, represents the first attempt to comprehensively evaluate the neurological disease admission burden in the country using a dedicated inpatient sample. To our knowledge, this is the first study in Somalia focusing exclusively on hospitalized patients with neurological disorders. Despite its modest sample size, the study offers valuable insights into the patterns of neurological diseases and their outcomes in a low-resource setting. Neurology remains a relatively underdeveloped and underrepresented medical specialty in Somalia. In many regions of the country, access to specialized neurological care is extremely limited, and the specialty itself is neither widely practiced nor well understood. Consequently, data on the epidemiology and clinical profile of neurological illnesses are sparse, particularly in inpatient settings.
The pattern and distribution of neurological disorders among hospitalized patients differ across sub-Saharan Africa. A study in Nigeria reported that neurological admissions constituted approximately 24.2% of all hospitalizations14. Similarly, a study in an Ethiopian city found neurological diagnoses in 18% of inpatients15. In Central Ghana, Sarfo et al. reported that 15% of admitted patients had neurological conditions, with stroke comprising the majority (54%) and central nervous system (CNS) infections accounting for 27%16. In contrast, the frequency and prevalence of neurological disorders in Somalia remain largely unknown. Most existing data come from outpatient-based studies, which may not accurately reflect the true burden or severity of neurological conditions requiring hospitalization. The current study addresses this gap by providing a descriptive analysis of neurological admissions and intrahospital mortality in a Somali tertiary care context. It is important to note that this study focused exclusively on patients admitted to the neurology department, and thus, the findings do not encompass the full neurological disease burden across the hospital. Some neurological conditions may be managed in emergency, internal medicine, or intensive care departments without formal admission to neurology, potentially leading to underestimation of certain diagnoses. Additionally, the outpatient population—which may exhibit different patterns of disease—is not represented in this sample. Nevertheless, the study establishes an important foundation for understanding neurological illness in Somalia, and the findings can guide both clinical and policy-level interventions aimed at improving neurological care and outcomes in similar low-resource settings.
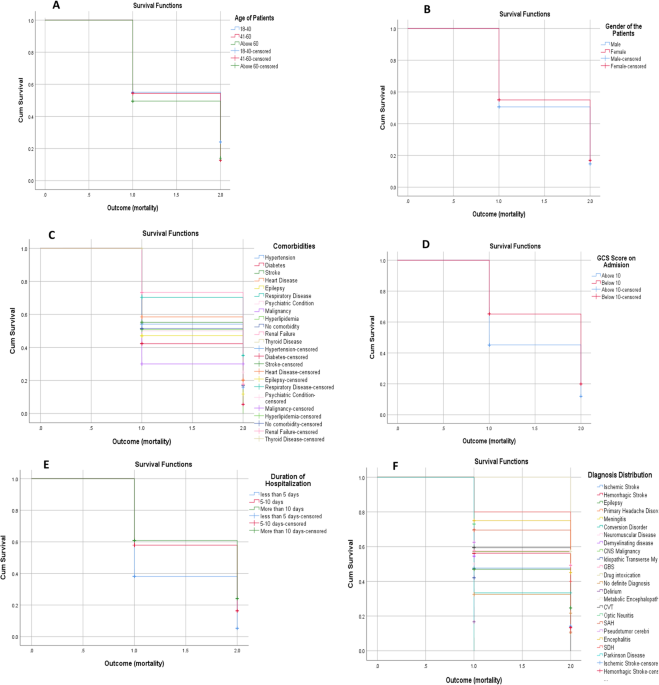
In our study, cerebrovascular disorders represented the majority of neurological diagnoses, with ischemic stroke accounting for 42% and hemorrhagic stroke for 26% of cases. These were followed by epileptic disorders, cerebral venous thrombosis (CVT), Guillain–Barré syndrome, subarachnoid hemorrhage, and demyelinating disorders. CNS infections constituted only a small proportion of neurological admissions, reflecting a shift in disease burden. This pattern aligns with earlier predictions that non-communicable diseases (NCDs) would rise in developing countries, accompanied by increasing mortality rates from these conditions17,18,19,20. Despite CVT and SAH are recognized subtypes of cerebrovascular disease but were reported separately in this study due to their distinct epidemiological and clinical features. This approach isadopted to highlight their unique clinical profiles, especially in younger and high-risk populations.
The demographic profile of patients further supports this shift: cerebrovascular disorders were more common in older adults, particularly those over the age of 60, and in males. These same groups also had the highest prevalence of comorbidities, including hypertension, diabetes, and heart disease. Epilepsy, which accounted for 7.8% of cases, was the next most frequent diagnosis and was notably more common among younger patients. Interestingly, our study observed a relatively high number of admissions for cerebral venous thrombosis (CVT), comprising 6.5% of cases. The majority of CVT patients were young women, typically in the peripartum period, many of whom had received inadequate antenatal care. The relatively high prevalence of cerebral venous thrombosis in our cohort—accounting for 6.5% of all neurological admissions may reflect a combination of referral bias, growing clinical awareness, and possibly underlying undiagnosed thrombophilic conditions, particularly in younger women. Additionally, in the absence of universal access to prenatal care and thromboprophylaxis protocols, some of these cases may represent the cumulative impact of systemic gaps in maternal health services.
Other neurological disorders such as peripheral neuropathies, CNS malignancies, motor neuron diseases, primary headache disorders, neuromuscular junction disorders, and neurodegenerative diseases were diagnosed less frequently. A small subset of patients (n = 40) remained undiagnosed due to limitations in neurocritical care expertise and the unavailability of advanced diagnostic tools. This highlights a critical gap in neurological care capabilities between high-income and low-resource settings. Effective management of acute neurologic illness (ANI) often depends on timely access to specialized investigations and critical care, which remains a major challenge in many low- and middle-income countries. Globally, the burden of NCDs has been increasing due to aging populations and lifestyle-related exposure to cardiovascular risk factors. Improvements in the treatment of infectious diseases have further shifted the epidemiology of acute neurological illnesses toward chronic, non-communicable etiologies21. In this context, our findings reflect the evolving pattern of neurological admissions in resource-limited settings, where traditional infectious causes are increasingly being replaced by stroke and other vascular conditions.
Globally, neurological disorders contribute significantly to the burden of disability-adjusted life years (DALYs), with stroke alone accounting for nearly half of this burden22. Stroke is the second leading cause of death worldwide and the foremost cause of long-term disability23. The risk of death following a stroke is approximately 50% higher in low- and middle-income countries (LMICs) compared to high-income countries (HICs). Moreover, over 58% of all strokes and 67% of stroke-related deaths occur in LMICs annually24. These disparities in outcomes are largely attributed to differences in prehospital care, the availability of neurosurgical interventions (e.g., decompressive hemicraniectomy), and access to evidence-based acute stroke therapies such as thrombolysis and endovascular thrombectomy25. In LMICs, stroke survivors often endure a disproportionately high burden of long-term disability due to the limited or absent rehabilitation services required for optimal recovery26. The increase in stroke-related mortality in LMICs may also be linked to inadequate adherence to established stroke care guidelines. For example, the INTERSTROKE study reported that the average time to neuroimaging (CT or MRI) in African centers was 30 h, with only 2.4% of patients undergoing vascular imaging and just 10% receiving transthoracic echocardiography27,28. These delays and omissions in essential diagnostics reflect the systemic gaps in stroke care across the region. In Somalia, stroke care is particularly challenged by a fragile healthcare infrastructure that has been severely undermined by decades of conflict. The country faces a critical shortage of trained healthcare professionals, essential medical supplies, and financial support mechanisms for medical treatment. Only a few hospitals nationwide are equipped to manage acute stroke cases, and currently, there are no dedicated stroke units in operation. Furthermore, surgical management options for stroke, when indicated, are constrained by both limited technical capacity and a lack of skilled personnel. Stroke management protocols, though available, are applicable in only a small number of facilities. Emergency services are poorly organized; ambulance systems are largely absent, forcing patients to rely on private or informal transport to reach medical facilities. These delays in prehospital care, combined with the lack of acute intervention and post-stroke rehabilitation, contribute to the high stroke-related mortality and disability observed in Somalia29.
Epilepsy poses a significant burden in sub-Saharan Africa, shaped by a complex interplay of limited healthcare infrastructure, cultural beliefs, and socioeconomic constraints. In Somalia, the true prevalence of epilepsy remains unknown, as there are no nationwide epidemiological studies assessing its burden or distribution. In our study, all patients diagnosed with epilepsy were admitted due to status epilepticus. Notably, the majority of these individuals had a prior diagnosis of epilepsy and were already prescribed antiseizure medications. However, their admissions were primarily triggered by poor adherence to medication regimens, leading to seizure escalation and emergency presentations. These findings are consistent with a study by MS Hassan and colleagues in Somalia, which identified non-compliance with antiseizure drugs as the most common cause of status epilepticus presentations in emergency departments11. Similar trends have been observed across sub-Saharan Africa, where studies have reported poor compliance rates ranging from 37% in Ethiopia to 54% in Kenya and 67% in Nigeria30,31,32. Like Somalia, the key drivers of poor medication adherence in these regions include limited public awareness, pervasive stigma surrounding epilepsy, and financial barriers to consistent treatment access.
The primary limitation of this study is its hospital-based design. The spectrum of neurological conditions observed in teaching or tertiary institutions may not accurately reflect the prevalence or distribution of neurological diseases in the general population. Furthermore, this study included only patients admitted to the neurology department; individuals treated in the outpatient clinic were not assessed. As a result, the neurological disease patterns among outpatients—potentially presenting with less severe or diagnostically distinct conditions—were not captured. Despite these limitations, the study offers important strengths. The hospital where the research was conducted functions as a national referral center, receiving patients from across the country. Therefore, while not population-based, the sample is likely to provide a valuable and reasonably representative insight into the burden of neurological admissions in Somalia. Moreover, the findings accurately reflect the types of neurological disorders most frequently encountered by neurologists in the country, offering a foundational reference point for future research, resource planning, and training needs.
İn conclusıon, This study represents the first comprehensive hospital-based assessment of neurological admissions in Somalia and reveals that cerebrovascular diseases—particularly ischemic and hemorrhagic stroke—are the leading causes of neurological hospitalization, followed by epileptic disorders and cerebral venous thrombosis. The high in-hospital mortality rate (23%) was significantly associated with older age, presence of comorbidities, low Glasgow Coma Scale scores, ICU admission, and longer hospital stays. Notably, cerebral venous thrombosis was disproportionately observed among young women, reflecting both demographic and systemic healthcare factors. These findings underscore the urgent need for context-specific strategies to improve stroke care, enhance early recognition of neurological emergencies, and strengthen neurology services in resource-limited settings. Addressing gaps in maternal health, expanding access to diagnostic tools, and investing in specialized neurology training are essential to reducing the burden of neurological morbidity and mortality in fragile health systems like Somalia’s.
link