Factors contributing to family resilience in the context of schizophrenia: a descriptive qualitative study | BMC Psychiatry

We invited 25 individuals to participate in the study; of these, 23 consented, comprising 18 patients and 5 family caregivers. The reasons for non-participation included time constraints for 1 caregiver and a lack of interest from 2 patients. The study involved participants with a mean age of 46.2 years (range: 18–67 years). Specifically, patients had a mean age of 47.1 years, whereas family caregivers had a mean age of 43.2 years. Most participants (42.4%) came from extended families, while 24.2% were part of nuclear families, and the remainder belonged to single-parent households. Additionally, 80% of caregivers lived in the same household as the patients, facilitating direct caregiving interactions, while 20% lived separately and relied on alternative support systems. The average self-assessed Family Warmth Level among participants stood at 6.9 points, while the FRAS-C score averaged 98.4 points. Notably, urban participants (n = 14) emphasized professional support systems and medical resources more frequently than rural participants (n = 9), who highlighted familial bonds and religious faith. Extended families demonstrated stronger support networks but also reported more complex communication challenges compared to nuclear families. The characteristics of participants refer to Table 1.
Understanding of family resilience
Before presenting the main themes, it is important to note participants’conceptualization of family resilience. When asked about their understanding of this concept, participants described it using various metaphors and experiences:
“Family resilience is like a big tree—when storms come, the branches may bend but the roots hold firm. Our family bends with my illness but doesn’t break.” (P8).
“It means we can bounce back. Every time he has an episode, we fall down, but we get up again, maybe a bit stronger in knowing what to do next time.” (C8).
“For me, resilience is when my family doesn’t give up on me even when I give up on myself. They keep believing things can get better.” (P6).
These conceptualizations revealed a shared understanding between patients and caregivers that family resilience involves persistence, mutual support, and the ability to adapt and learn from challenges. This common ground provided a foundation for exploring the factors that influence this resilience (Table 2).
The study outcomes are encapsulated within Walsh’s Family Resilience Framework, comprising three primary themes: Family Organization and Resources, Family Belief, and Family Communication. Within these overarching themes, our analysis revealed 12 sub-themes (Fig. 1). As illustrated in Fig. 1, these themes do not exist in isolation but interact dynamically. The circular arrangement emphasizes their interconnected nature, with bidirectional arrows indicating mutual influences. For instance, adequate financial resources (Family Organization) can foster hope (Family Belief), which in turn enhances communication willingness (Family Communication). Conversely, family conflicts can deplete resources and diminish hope, creating negative feedback loops that challenge resilience.
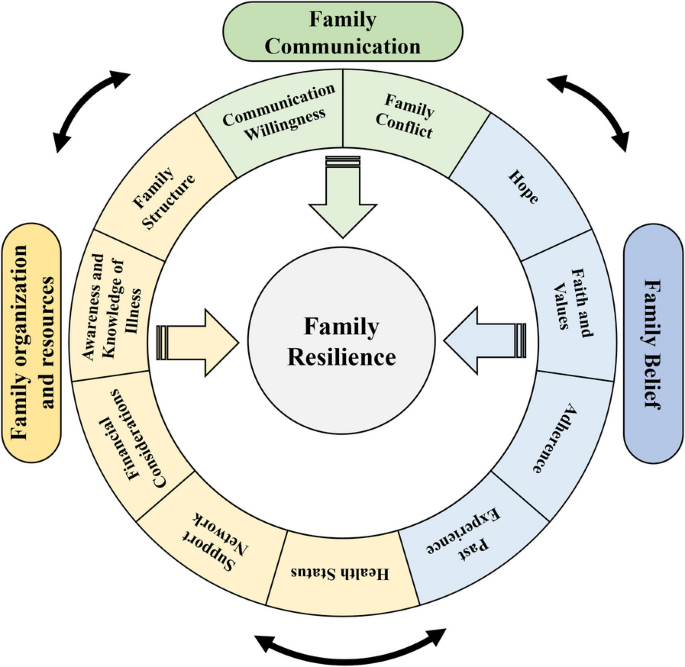
The influencing factors of family resilience in patients with schizophrenia based on Walsh’s Family Resilience Framework
Theme 1: family organization and resources
This theme encompasses five subthemes: Family Structure, Awareness and Knowledge of Illness, Financial Considerations, Support Network, and Health Status. These organizational factors form the structural foundation upon which family resilience is built, providing the tangible and intangible resources families draw upon when facing schizophrenia-related challenges.
Subtheme 1.1: family structure
Participants reported diverse family dynamics that influenced their experiences of support and resilience in coping with schizophrenia. Family fragmentation, shifting priorities, and caregiver roles emerged as central themes in the accounts. The impact of family structure on resilience was particularly evident in how it affected the distribution of caregiving responsibilities and emotional support.
“My parents are divorced and live separately. They often fight with each other and with me. I don’t feel loved by them… Even when I’m sick, they don’t seem to bother about me.” (P3)
This quote illustrates how family fragmentation directly undermines the patient’s sense of being supported, a fundamental component of family resilience. The absence of unified parental support creates an environment where the patient feels isolated in managing their illness. Similarly, the challenges of caregiving were highlighted by participants from fractured family environments, where responsibilities were unevenly distributed or unsupported.
“He’s always getting into fights with people and can’t hold down a job. His mom doesn’t look after him either—she up and left. I don’t have time to deal with him since I work out of town and only come back once a year.” (C12)
Rural participants like C12 faced additional challenges due to work-related migration, a common phenomenon that fragments family support systems and leaves patients with minimal consistent care. Some participants noted shifts in family attention and care priorities, particularly after major life events such as childbirth.
“Before giving birth, I was the center of attention in my family. However, after having the child, there isn’t as much time to take care of me anymore. Everyone is focused on the child, so I don’t receive the same level of care as before.” (P17)
This shifting of priorities represents a critical juncture where family resilience can be tested, as resources—both emotional and practical—are redistributed, potentially leaving the patient feeling marginalized. Caregivers also described the demands of balancing competing responsibilities and the lack of adequate support systems, particularly in families where one caregiver was expected to manage most of the workload.
“Kids have so many direct needs—you gotta take care of their eating, drinking, pooping, peeing, the whole shebang. Her husband is out working all day every day, so there’s nobody there to give her a hand or a break.” (C11)
In contrast, participants from stable extended families reported stronger resilience:
“Even though we’re not rich, our family is complete. My parents, my sister, we all live together and share the responsibility. When I’m having a bad day, someone is always there.” (P11)
Subtheme 1.2: awareness and knowledge of illness
Participants shared varying levels of understanding regarding schizophrenia, which influenced their experiences with the illness and interactions with family members. Knowledge emerged as a critical resource that could either facilitate or hinder family resilience. Some patients described a strong awareness of their condition, which fostered collaboration and support within their families:
“I know what causes it, I also know how to control it, so my family is happy to face the disease together with me.” (P2)
This patient’s knowledge empowers both themselves and their family, transforming the illness from an unknown threat to a manageable challenge, thereby strengthening collective resilience. Other participants discussed challenges when family members or patients themselves did not fully acknowledge or understand the illness. For example, one caregiver expressed frustration with their daughter’s denial of her condition:
“She (daughter) still doesn’t admit that she is sick…She refused our help, we don’t have a good way to help her.” (C4)
Denial creates a fundamental barrier to resilience by preventing the family from mobilizing appropriate resources and support strategies. This was more common among younger patients and those from rural areas with limited mental health literacy. Patients also noted that while their families were supportive, a lack of knowledge about the illness led to feelings of being misunderstood:
“My family cares about me and treats me well, but they don’t understand my condition very well. They will never know what I want!” (P5)
This disconnect between care and understanding highlights how emotional support alone may be insufficient without accompanying knowledge, potentially limiting the family’s ability to provide targeted assistance. Caregivers described initial difficulties in recognizing schizophrenia, sometimes misinterpreting symptoms as personality traits or behavioral issues:
“We didn’t know what was wrong with him…we thought he was just stubborn and didn’t want to listen to us.” (C5)
Urban families generally demonstrated better illness awareness, often attributing this to greater access to mental health information and services. One urban caregiver noted:
“Once we got the diagnosis, I spent hours online learning about schizophrenia. Now I can recognize early warning signs and we’ve prevented several relapses.” (C14)
Subtheme 1.3: financial considerations
Participants frequently highlighted financial difficulties as a significant factor impacting their management of schizophrenia. Financial resources intersected with every other aspect of family resilience, from accessing treatment to maintaining family stability. Many patients and caregivers described economic challenges, including the inability to afford medication or the financial strain of treatment expenses.
Some patients noted that their family’s financial instability directly affected their access to necessary medications:
“I can’t afford the medication, our family is very poor, my father also does not have a stable job.” (P3)
The inability to afford consistent medication creates a cycle where untreated symptoms lead to greater disability, further reducing the family’s economic capacity and resilience. Caregivers expressed similar concerns, emphasizing the limitations of financial support systems, such as rural health insurance, and the broader impact of these challenges on family resilience:
“The rural health insurance only covers half of the patient’s treatment costs. The expenses are putting a huge strain on me. My family is constantly arguing about money. It’s just so stressful, you know?” (C10)
Financial stress emerged as a primary source of family conflict, illustrating how economic pressures can undermine communication and mutual support—key components of resilience. Rural families were particularly vulnerable, with limited insurance coverage and fewer employment opportunities. In contrast, financially stable families described how economic security enhanced their resilience:
“Because we have savings and good insurance, we can focus on recovery rather than worrying about the next prescription. It makes all the difference.” (C7)
Subtheme 1.4: support network
Participants described varying experiences regarding the role of their family and social networks in providing support in the context of living with schizophrenia. Support networks functioned as external resources that could either amplify or compensate for internal family resources. While some individuals reported strong family support, others highlighted the challenges of stigma and isolation.
“My family is always concerned about my condition. They support and understand me. They never scold or blame me for my illness. Whenever I’m feeling down, they’re there to encourage and comfort me. I’m not fighting this battle alone.” (P6)
This comprehensive support system exemplifies how emotional, practical, and social support combine to create an environment conducive to resilience, where the patient feels valued and integrated rather than burdensome. Conversely, other participants described social stigma as a barrier to accessing support. This stigma often extended to the family, influencing their interactions with the broader community.
“People look down on us, saying we have a crazy woman in our family. I’m afraid to go out and face others. I only take her to see the doctor at night when there are fewer people around.” (C6)
Stigma effectively shrinks the family’s support network by creating social isolation, forcing families to rely solely on internal resources which may already be strained. This was particularly pronounced in rural communities where mental health stigma remained strong. Urban participants more frequently mentioned professional support networks:
“Our doctor connected us with a family support group. Meeting other families going through the same thing has been invaluable—we share tips, encouragement, and sometimes just understanding.” (C1)
Subtheme 1.5: health status
Participants highlighted the complex interplay between their own health conditions and the health of their caregivers, revealing additional layers of vulnerability and strain in families affected by schizophrenia. Health status emerged as both a resource and a constraint, with family members’physical and mental well-being directly impacting their capacity to provide care and maintain resilience.
“A few years ago, I wanted to send the patient to the hospital, but being an elderly lady with my own health problems, I didn’t have any means to persuade him to come to the hospital.” (C4)
This illustrates how compromised caregiver health creates practical barriers to accessing treatment, potentially leading to crisis situations that further strain family resilience. In some cases, participants noted the compounded challenges when multiple family members were affected by mental or physical health issues, further diminishing the family’s capacity to provide consistent care and support.
“My mom also has a mental illness, and she’s even worse than me. My dad is the only one holding this family together. To be honest, I’m really worried that one day he might not be able to cope with it anymore.” (P17)
The concentration of caregiving responsibility on a single healthy family member creates a precarious situation where the family’s entire support structure depends on one person’s continued well-being, representing a significant vulnerability in the family’s resilience.
Themes 2: family belief
This theme includes four subthemes: Hope, Faith and Values, Adherence, and Past Experience. Family beliefs serve as the cognitive and emotional framework through which families interpret and respond to schizophrenia-related challenges, profoundly influencing their resilience strategies.
Subtheme 2.1: hope
Participants articulated diverse perspectives on hope in the context of managing schizophrenia, encompassing both feelings of despair and aspirations for the future. Hope emerged as a dynamic force that could either energize or deplete family resilience, often fluctuating with the illness trajectory.
“I have no hope for his situation anymore. This disease is incurable, and he’s just a burden. I’m starting to not care about him anymore.” (C5)
“I feel like there is no hope for my future anymore. I think everything my family has done for me is useless. This disease can’t be cured.” (P4)
These expressions of hopelessness reveal how prolonged exposure to the challenges of schizophrenia can erode the emotional resources necessary for resilience, leading to disengagement and fatalism. This was more common among families who had experienced multiple relapses or treatment failures. Conversely, some participants expressed a strong sense of optimism and determination to overcome their illness, emphasizing personal goals and the support received from their families.
“I want to recover from my illness and live a happy life in the countryside… I hope to get married someday and have a child. So I won’t back down, my family has already helped me a lot, I don’t want to let them down.” (P6)
This future-oriented hope, anchored in specific life goals and reciprocal family commitment, demonstrates how hope can motivate both patient and family members to persist despite challenges, thereby maintaining resilience. The source and nature of hope varied between urban and rural participants. Urban families often placed hope in medical advances and professional treatment:
“The doctor told us about new medications coming out. We keep hoping one of them will work better for our son.” (C3)
While rural families frequently drew hope from traditional or spiritual sources:
“We believe that with Buddha’s blessing and our persistence, things will improve slowly.” (C9)
Subtheme 2.2: faith and values
Participants described how their faith, personal values, and family beliefs influenced their experiences with schizophrenia. These belief systems provided meaning-making frameworks that helped families contextualize and cope with the illness. Some found comfort and improvement through religious practices.
“After I got sick, my mom and sister started taking me to Buddhism. They said that Buddha and the Bodhisattvas are the best tranquilizers… I feel my illness is improving a lot, and it’s quite helpful.” (P18)
Religious faith offers both practical coping strategies (meditation, community support) and existential comfort, helping families maintain resilience by providing a sense of control and meaning in the face of uncertainty. This was particularly prominent among Buddhist and Christian participants. Trust in professional caregivers provided reassurance for some families.
“The head of the department assured me that treating patients is their responsibility and duty. I feel very relieved, so our family entrusted the patient to the hospital with full confidence.” (C3)
This trust in medical authority represents a secular form of faith that enables families to share the burden of care, preserving their emotional resources for other aspects of resilience. Several participants faced negative perceptions and lack of support from family members.
“My grandmother did not like me, because my mother was from a different province, she always said I was a bastard… she always beat and scolded me…” (P1)
Negative family values and discrimination within the family system directly undermine resilience by creating internal conflicts and denying the patient fundamental emotional support. For others, familial responsibilities and values motivated them to cope with their condition.
“Because I am the patient’s mother, and I have to take responsibility for her.” (C4)
“My dad has sacrificed a lot for me. He says as a father, he will never give up on his son. I want to take care of him; he’s getting old, so I must focus on getting well.” (P6)
These expressions of mutual obligation and filial piety, deeply rooted in Chinese cultural values, create powerful motivations for both caregiving and recovery, strengthening family bonds and resilience.
Subtheme 2.3: adherence
Participants described varying experiences with medication adherence, influenced by individual behaviors and family involvement. Adherence represented a behavioral manifestation of family beliefs about treatment and their collective capacity to manage the illness. Some caregivers expressed frustration with the challenges of ensuring consistent medication use.
“When we make him take medicine, he hides it or throws it up. I’ve found it several times when I’m cleaning, like under the sofa, in the toilet. How should I deal with him?” (C5)
Non-adherence challenges the family’s sense of efficacy and control, potentially leading to conflict and reduced resilience as family members feel their efforts are futile. In contrast, other participants reported long-term adherence to prescribed treatments, often facilitated by family support and encouragement, despite initial difficulties.
“I’ve been taking medicine for over ten years, and I’m used to it. At the beginning, the side effects were quite severe, and I didn’t want to take it. But I listened to my mom and stuck with it, and now there’s nothing wrong.” (P11)
Successful long-term adherence, achieved through persistent family support, demonstrates how families can overcome initial challenges to establish stable treatment routines that enhance overall resilience.Families that integrated medication into daily routines showed better adherence:
“We made it part of breakfast—pills with porridge every morning. Now it’s just automatic, no arguments needed.” (C13)
Subtheme 2.4: past experience
Participants shared how their past experiences, either personal or within their family, influenced their approach to managing schizophrenia and seeking support. Past experiences served as a repository of learned strategies and emotional responses that shaped current resilience patterns. Some caregivers recounted how their own experiences with mental health shaped their vigilance and decision-making regarding family members.
“I have a mental condition too… but once I start taking medication, everything will be fine. So when I noticed my brother showing symptoms of suspected mental illness, I immediately took him to see a doctor.” (C2)
Personal experience with mental illness provides both practical knowledge and reduced stigma, enabling quicker recognition and intervention that can prevent crisis situations and maintain family stability. For others, past episodes of instability highlighted the consequences of interruptions in treatment or external triggers that led to relapse.
“Actually, my condition was already stable, but one day I remembered my ex-husband and I went out to drink for five days straight, not coming home. My family couldn’t find me. Those five days, I didn’t take my medication, and the illness relapsed.” (P14)
This experience illustrates how past crises become cautionary tales that inform current vigilance and preventive strategies, with families learning to recognize and avoid triggers that threaten stability. Families with multiple experiences of recovery demonstrated enhanced resilience:
“We’ve been through three major relapses now. Each time we learn something new—warning signs, what works, what doesn’t. We’re like experts now!” (C15)
Themes 3: family communication
This theme comprises two subthemes: Communication Willingness and Family Conflict. Communication serves as the primary mechanism through which family resources and beliefs are mobilized and coordinated, making it essential for operationalizing resilience.
Subtheme 3.1: communication willingness
Participants shared contrasting perspectives on communication within the family, highlighting differing levels of openness and mutual engagement. The willingness to engage in open dialogue determined whether families could effectively share burdens, coordinate care, and maintain emotional connections. Some caregivers described challenges in fostering communication, noting reluctance or emotional barriers from the patients.
“I don’t want to tell them my troubles, they won’t listen. They just want to send me here, to get me out of their sight.” (P3)
This perception of being unheard or unwanted creates a communication breakdown that isolates the patient and prevents the family from understanding and addressing their needs, directly undermining resilience. From the caregiver’s perspective, this reluctance was often interpreted as avoidance or distrust.
“He shuts himself in his room and doesn’t talk to anyone, no matter how much we try. It feels like he’s building a wall between us.” (C9)
The metaphor of walls captures how communication barriers create emotional distance that fragments the family unit, preventing the coordination and mutual support essential for resilience. In contrast, some participants reported open and supportive dialogue that facilitated mutual understanding and strengthened family bonds.
“I keep in touch with my son, my mother, my brother, they all care about me, I also appreciate them. I talk to them about my thoughts, my feelings, they will listen, and also give me advice.” (P12)
This reciprocal communication creates a supportive feedback loop where expression is met with validation and assistance, reinforcing family cohesion and collective problem-solving capacity. Caregivers in these scenarios described efforts to actively engage the patient, offering a consistent and patient-focused approach.
“I always make time to sit with him and talk. Even if it’s just small things, I think it helps him feel less alone.” (C14)
Proactive communication efforts demonstrate how families can overcome initial barriers through persistence and unconditional availability, gradually rebuilding trust and openness. Communication patterns differed notably between family structures. Nuclear families reported more direct communication:
“With just the three of us, we have family meetings every week to check in. It keeps everything in the open.” (C8)
While extended families faced more complex communication dynamics:
“With so many people involved, messages get confused. Sometimes grandma tells him one thing, I say another… it’s chaos.” (C11)
Subtheme 3.2: family conflict
Participants described family conflicts as a significant factor influencing the experience of resilience within families managing schizophrenia. Conflict emerged as both a symptom of strained resilience and a factor that further depleted family resources. Tensions within family relationships were commonly reported, with disagreements often centered on caregiving responsibilities or financial matters.
“My sister-in-law…she often argues with me, for money, for other things. She does not care about my illness, nor does she help me, she also influences my brother, makes him treat me badly.” (P16)
Extended family conflicts create alliance patterns that can isolate the patient and divide available support, transforming potential resources into sources of additional stress. Caregivers in these situations reported the added challenge of managing the patient’s mental health while navigating unresolved family dynamics.
“My husband and I argue all the time. It’s hard to focus on my daughter when we can’t agree on anything about her care.” (C8)
Marital conflict specifically undermines the parental subsystem’s ability to provide consistent, coordinated care, creating an unstable environment that impedes recovery and family resilience. However, some families demonstrated conflict resolution strategies that strengthened resilience:
“We used to fight about everything—medication, money, whose fault it was. Then we started seeing a family counselor. Now we have rules: no blame, focus on solutions. It’s made such a difference.” (C1)
The interplay between themes
Throughout the interviews, participants’narratives revealed how the three main themes—Family Organization and Resources, Family Beliefs, and Family Communication—continuously influenced each other. For instance, P6’s story exemplifies this interaction: his family’s stable structure and adequate financial resources (Organization) fostered hope for recovery and strong family values of mutual support (Beliefs), which in turn facilitated open communication about his needs and progress (Communication). This positive cycle strengthened their overall resilience.
Conversely, P3’s experience illustrates negative interactions: parental divorce and poverty (Organization) led to hopelessness and feelings of being unloved (Beliefs), resulting in communication breakdown and isolation (Communication). These negative spirals were particularly evident in families facing multiple stressors.
Urban–rural differences added another layer to these interactions. Urban families typically had better access to professional support and information (Organization), which informed more medicalized beliefs about treatment (Beliefs) and structured communication patterns around medical management. Rural families relied more heavily on extended family networks and spiritual resources, leading to different configurations of resilience factors but not necessarily less effective outcomes.
link






