Psychosocial determinants of oral health-related quality of life in periodontitis patients
This study is the first to investigate the intricate interactions among self-efficacy for oral care, OHRKAP, SES, perceived social support, and OHRQoL in patients with periodontitis. In this study, the mean OHIP-14 score for patients with periodontitis was 14.20 ± 9.19. A study conducted by Machado et al.8 revealed an OHIP-14 score of 9.5 ± 11.3 in Portuguese respondents. Additionally, research by Fuller et al.41 indicated that the OHIP-14 score for patients with chronic periodontitis was 12.9 in London, compared to 6.6 in the healthy population. In contrast, Chinese patients with periodontitis may experience diminished quality of life regarding dental health. Given the influence of varying national contexts, cultural backgrounds, and patient demographics, this study advocates for a comprehensive analysis of oral health-related quality of life and its direct and indirect effects in patients with periodontitis, depicting the intricate interconnections involved in this relationship.
The current findings underscore that oral health-related knowledge, attitude, self-efficacy, and socioeconomic status are strongly and negatively associated with OHRQoL. In other words, patients with periodontitis who exhibited superior knowledge, attitude, and practice levels, together with elevated self-efficacy and socioeconomic status, demonstrated reduced OHRQoL scores, indicating an enhanced oral health quality of life. The direct effect of self-efficacy was the most substantial, at 60%, aligning with the findings of several previous studies. A study of Chinese college students identified self-efficacy as a fundamental component affecting OHRQoL among this demographic42. Allen et al.43 indicated that those with diminished self-efficacy exhibited elevated disease levels, increased gingival bleeding scores, and reduced satisfaction regarding their oral health. Additionally, recent research suggests that mobile health applications designed for periodontal health, when incorporating features to enhance self-efficacy, can significantly influence how individuals manage their dental and gum health. The findings on self-efficacy should also serve as the foundation for the development of artificial intelligence-based digital monitoring systems and self-efficacy assessment tools44,45.
The cultivation of self-efficacy is a protracted process shaped by multiple factors, such as individual experiences, verbal feedback, and social support. Previous research indicates that social support indirectly impacts OHRQoL among Chinese college students by affecting self-efficacy and various multidimensional factors, including knowledge, attitudes, and practices42. This study reconfirms that subjective social support (PSS) significantly influences self-efficacy. Simultaneously, PSS can act as a mediator of the effects of socioeconomic status on self-efficacy. It is presumed that this has practical value in buffering the adverse effects of low socioeconomic status and enhancing mental health. This is in line with the research conducted by Huang et al. regarding college students during the COVID-19 closure46. Secondly, the mediation pathways identified suggest that subjective social support exerts an indirect influence on OHRQoL by impacting self-efficacy (82%); additionally, social support can also indirectly impact OHRQoL through OHRKAP (18%). Research indicates that social support can be improved through two main areas23. First, instrumental support, such as social and medical security systems, pensions, and financial assistance for child-rearing expenses, is provided. Second, emotional support can alleviate the emotional stress of patients with chronic diseases. For example, community health education activities and regular check-ups for patients with periodontal disease can reduce their concerns about their physical condition. As a dimension of family support, good emotional expression can reduce patients’ feelings of guilt regarding the economic burden of their illness and the burden of caring for their children. However, current policy guidance lacks recommendations for this crucial socioeconomic sector.
The Knowledge, Attitudes, and Practices (KAP) theoretical model has been thoroughly examined in relation to oral health-related quality of life. Oral health-related knowledge, attitudes, and practices were incorporated as variables in the SEM, thereby decreasing the number of variables, streamlining the model structure, and introducing methodological innovation. The findings of this research indicated a substantial correlation between OHRKAP and OHRQoL, suggesting that those with elevated OHRKAP levels experience an improved oral health-related quality of life, similar to the results of Zheng et al.18. A study examining the current status of periodontal health knowledge, attitudes, and practices among Chinese adults16 indicated that such variables were correlated with gender, age, education, income, smoking habits, and history of periodontal disease. This study revealed that socioeconomic status and perceived social support were significantly and positively associated with the OHRKAP. Furthermore, perceived social support can mitigate the influence of socioeconomic status on OHRKAP through mediation. Specifically, patients from disadvantaged socioeconomic backgrounds generally receive less financial assistance and are more likely to possess poor oral health-related knowledge, attitudes, and practices. In this context, social support functions as a moderating buffer, mitigating the effects of socioeconomic disparities on OHRKAP among patients with periodontal disease. This is similar to prior research26, which found that social support is vital in buffering the impacts of SES and cognitive capacities associated with an aging population.
In addition, the total score for oral health care knowledge, attitudes, and practices among periodontal patients was 39.04 ± 10.33, categorizing it within the low to medium level. A cross-sectional study revealed that knowledge, attitudes, and practices regarding periodontal health among Chinese individuals were predominantly insufficient, with less than 20% of participants exhibiting an understanding of periodontal disease16. Periodontal health initiatives should be advocated for the entire adult population, with particular emphasis on older adults, individuals with lower educational attainment, and those from lower-income backgrounds.
A positive association between socioeconomic status (SES) and health has been well documented47. This association has been established for socioeconomic status indicators at both the individual level48 and the societal level49 across nearly all health outcomes, including mortality, morbidity, and disability50. In this study, SES, while highly correlated with OHRQoL, also had a favorable impact on two psychosocial factors: self-efficacy and perceived social support. In other words, having a higher SES usually results in more economic assistance, more social support, greater self-confidence, and a higher quality of life. Similar findings were discovered in Ting Ge’s study, which revealed that individuals with a high socioeconomic status are typically thought to have more financial support, positive family, friends, and social support, and thus more life satisfaction and pleasant emotional states51.
Additionally, numerous mediating pathways between SES and OHRQoL were identified. Socioeconomic status (SES) exerted an indirectly influenced OHRQoL through multiple mediating effects of perceived PSS, oral health knowledge, attitudes, and practices (OHRKAP), and self-efficacy. SES affected the quality of life and OHRKAP of patients with periodontitis sequentially through perceived social support and self-efficacy. This may be attributed to unequal access to or control over material, property, social, and intellectual resources among patients with varying socioeconomic statuses52. This results in disparities in personal views and behavioral outcomes when confronted with a disease. Overall, the main findings suggest that SES is an important moderator of the OHRQoL. This study aimed to contribute to the dialogue on socioeconomic inequalities by elucidating the complex relationship between SES and OHRQoL among patients with periodontitis.
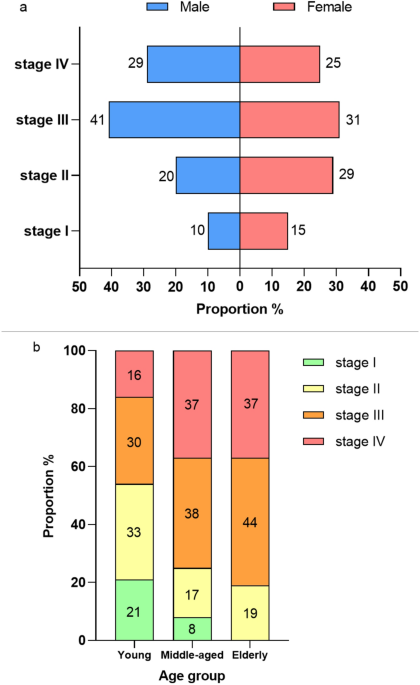
Furthermore, this study revealed that more females than males had periodontitis, which is inconsistent with previous findings that more males than females had periodontitis13. It is intriguing that the majority of female patients experienced mild to moderate periodontitis. The number of male patients was comparatively low; however, the majority of them experienced moderate to severe periodontitis (Fig. 1a). It can be considered that the possibility may be associated with factors such as pregnancy and hormonal alterations in women53. A prior study [54] indicated that women display more favorable attitudes toward dental visits, possess greater oral health knowledge, and are more aggressive in pursuing disease prevention than men. In contrast, men are more predisposed to pursue oral treatment for acute problems than women. Inadequate oral hygiene practices and increased tobacco consumption are significant factors contributing to the progression of periodontitis to moderate or severe stages by the time men seek treatment. Recent studies have indicated that men and women are not equally effective in using electronic health tools and participating in digital intervention measures, which may be one reason for the differences in oral health outcomes between the sexes [55].
Regarding age structure, young people have a higher rate of periodontal disease visits, with mild to moderate severity, while older adults have a lower frequency of periodontal disease visits and higher severity. The infrequent periodontal visits among the elderly, coupled with the high severity of periodontitis. This can be attributed not only to direct factors such as immune and cellular senescence and impaired wound healing, but also to indirect factors, including physical and cognitive impairments and limited access to care [56]. Given the challenges posed by China’s aging population, additional efforts to promote periodontal health in the elderly are essential.
Our study highlights that self-efficacy, perceived social support, and socioeconomic status significantly impact OHRQoL in patients with periodontitis, consistent with findings from international research. Evidence from Europe, North America, and Southeast Asia similarly indicates that psychosocial determinants, such as confidence in oral care practices and the presence of supportive social networks, play key roles in shaping oral health behaviors and outcomes. Although the pathways and effect sizes may differ across populations due to variations in healthcare access, cultural norms, and socioeconomic conditions, the overarching influence of psychosocial factors on oral health appears globally consistent. Notably, our structural equation model demonstrated that self-efficacy has the strongest direct effect on OHRQoL, while perceived social support functions as an important moderator, reflecting multi-country evidence on the value of empowerment and supportive networks in oral health management. These international comparisons contextualize our findings and underscore the potential benefits of interventions that enhance self-efficacy, reinforce social support, and address socioeconomic disparities to improve periodontal health and quality of life. Moreover, recognizing population-specific differences can guide tailored strategies for vulnerable groups, including the elderly and individuals with lower socioeconomic status, to optimize intervention outcomes.
This study provides important insights into the relationships among oral health knowledge, attitudes, practices, psychosocial factors, and oral health-related quality of life in patients with periodontitis. Additionally, our findings have important implications for multiple stakeholders. Researchers can build on these results to design targeted interventions aimed at improving oral health knowledge, attitudes, and practices. Public health practitioners and policymakers may use these insights to develop programs and strategies that enhance periodontal care and oral health literacy at the population level.
Limitations
Several limitations should be acknowledged. First, this study was conducted at a single center, which may limit the generalizability of the findings to broader populations. Second, our study included only patients diagnosed with periodontitis and did not incorporate a comparison group without the disease. Therefore, while the findings offer valuable information on factors influencing quality of life among affected individuals, they cannot directly assess determinants of disease occurrence. Third, the cross-sectional design of the study limits causal inference, and future research using longitudinal designs is warranted to clarify causal relationships. Fourth, more targeted questionnaires specifically addressing periodontal health knowledge, attitudes, and practices could enhance the precision of future studies. Finally, we employed a structural equation model to represent oral health knowledge, attitudes, and practices collectively, which simplified the analysis but may have overlooked potential interactions among these components.
link




